Not every broken tooth needs to be removed — sometimes, what remains is enough to rebuild
There is a moment that many patients remember very clearly — the moment they are told that a tooth cannot be saved and needs to be removed.
Being advised a tooth extraction often feels final. It usually comes after pain, a broken tooth, or repeated dental treatment, and the natural assumption is that there are no other options left.
For most people, the next step seems straightforward: remove the tooth and replace it with an implant or bridge.
But is tooth extraction always necessary?
This is one of the most common and important questions patients ask — especially when they are looking for an alternative to tooth extraction or wondering if there is any way to save a natural tooth without extraction.
In many cases, extraction is indeed the correct and safest treatment, particularly when the tooth is severely damaged, infected, or lacks adequate support.
However, there are also situations where a tooth that appears unsalvageable may still have the potential to be restored.
Over the years, we have seen several patients come to us after being advised tooth extraction elsewhere. While the recommendation is often clinically valid, it is not always the only possible solution.
With careful diagnosis, including radiographic evaluation and assessment of the remaining root and bone support, it is sometimes possible to explore options that help avoid tooth extraction and preserve the natural tooth.
This is especially relevant in cases where the visible portion of the tooth is broken, but the root structure remains intact.
In such situations, modern techniques allow us to rebuild the tooth using methods like post and core restorations and full-coverage crowns.
These approaches can restore function, maintain bone, and offer a more conservative alternative compared to extraction and replacement.
At the heart of this approach is a simple principle: whenever possible, preserving a natural tooth is always preferable to removing it.
A natural tooth maintains its original biomechanics, helps preserve surrounding bone, and often provides a more comfortable long-term outcome.
In this article, we will walk you through a real patient case where a tooth that was advised for extraction was successfully saved.
It highlights an important takeaway for anyone facing a similar situation — before proceeding with tooth extraction, it is worth understanding whether the tooth can still be preserved with the right diagnosis and treatment approach.
Understanding why tooth extraction is recommended
Being advised a tooth extraction can feel abrupt, especially when the immediate focus is on relief from pain or resolving a visible problem.
However, the recommendation for tooth extraction is usually not based on a single symptom or quick judgment.
It is a clinical decision made after evaluating whether the tooth can continue to function safely and predictably in the long term.
At its core, tooth extraction is recommended when a tooth can no longer be restored in a way that maintains health, stability, and comfort.
This typically happens when both the structure of the tooth and its supporting foundation are compromised beyond repair.
One of the most common reasons for tooth extraction is extensive structural damage.
When a tooth is severely broken or decayed to the point that there is insufficient healthy structure left to support a restoration, rebuilding it may be unreliable. In such situations, even if a temporary solution is possible, it may fail over time.
Recommending tooth extraction in these cases helps prevent repeated treatments and ongoing discomfort.
Another important reason is the condition of the root. The root acts as the anchor of the tooth within the bone. If the root is fractured, excessively short, or weakened in a way that affects stability, saving the tooth becomes unpredictable.
In these cases, tooth extraction is often the safest option, as it eliminates the risk of future complications.
Infection is another major factor. When an infection spreads deep into the tooth and surrounding structures, and cannot be controlled with treatments such as root canal therapy, tooth extraction may be necessary to prevent the infection from worsening.
This is particularly important when there are signs of swelling, abscess formation, or bone involvement.
Bone support also plays a critical role in the decision. A tooth relies on the surrounding bone for stability. When there is advanced bone loss — often due to gum disease — the tooth may become loose and unable to withstand normal chewing forces.
In such cases, tooth extraction is recommended not just to address the tooth itself, but to maintain overall oral health.
There are also situations where tooth extraction is advised as part of a broader treatment plan.
For example, in cases where adjacent teeth are affected, or where space needs to be created for proper alignment, removing a tooth may be necessary to achieve a better long-term outcome.
From a patient’s perspective, it is important to understand that recommending tooth extraction is not about choosing the quickest or easiest solution. It is about selecting a treatment that offers the most predictable and stable result over time.
In many cases, extraction followed by replacement — such as a dental implant or bridge — provides a reliable way to restore function and aesthetics.
At the same time, it is equally important to recognise that tooth extraction should not become the default response to every severely damaged tooth. There are situations where the tooth may still be salvageable, especially if the root and supporting structures are intact.
This is where a detailed evaluation becomes essential, helping determine whether tooth extraction is truly necessary or whether an alternative approach is possible.
This balance is what defines responsible dental care.
The goal is not to avoid tooth extraction at all costs, nor to proceed with it prematurely. The goal is to ensure that when tooth extraction is recommended, it is based on clear clinical need — and when it can be avoided, that opportunity is not overlooked.
For patients, this understanding is important. It shifts the perspective from simply accepting or resisting a recommendation to actively understanding the reasoning behind it.
And in some cases, it can open the door to exploring whether the natural tooth can still be preserved.
Tooth extraction or saving the tooth — making the right decision
Before we move into the case, it’s important to understand how dentists decide between tooth extraction and saving a natural tooth.
Many patients assume that once tooth extraction is advised, there are no other options left.
But in reality, the decision is often more nuanced — and in some cases, tooth extraction can be avoided with the right diagnosis and approach.
Tooth extraction becomes necessary when the tooth is no longer structurally or biologically viable. This typically includes situations where the root is severely fractured, where there is advanced bone loss around the tooth, or where infection has spread in a way that cannot be controlled.
In such cases, proceeding with tooth extraction is the safest and most predictable option. Attempting to save the tooth may lead to repeated complications, discomfort, and higher long-term costs.
However, there is another category of cases that often sits in a grey zone — and this is where many patients seek clarity.
These are situations where the visible portion of the tooth is severely damaged or broken, sometimes leaving behind only a root stump.
At first glance, such teeth are commonly advised for tooth extraction, followed by replacement with an implant or bridge. From a conventional perspective, this recommendation is understandable.
But the key question is not how much of the tooth is visible.
The real question is: Can this tooth still be saved without tooth extraction?
The answer depends on the condition of what remains beneath the surface.
A detailed evaluation is essential to determine whether tooth extraction is truly necessary. This includes assessing the root structure, surrounding bone support, and the presence or absence of infection.
An X-ray helps identify whether there are any periapical changes that indicate infection at the root tip.
The amount of bone around the tooth is evaluated to ensure it can support functional forces. The length and integrity of the root are also critical factors — because even if the crown is lost, a strong and stable root can often serve as a foundation for restoration.
When these conditions are favourable, it opens up the possibility of an alternative to tooth extraction.
In such cases, instead of removing the tooth, we can consider rebuilding it using techniques such as post and core restorations followed by a full-coverage crown.
This approach allows us to save a broken tooth without extraction, restoring both function and stability while preserving the natural root.
There are several advantages to avoiding tooth extraction when it is clinically appropriate.
Preserving a natural tooth helps maintain the surrounding bone. Once a tooth is removed, the bone in that area begins to shrink over time, which is why procedures like implants are often required to restore both the tooth and the lost support.
By avoiding tooth extraction, this bone loss can be minimised.
Additionally, saving the natural tooth eliminates the need for surgical intervention, which is a significant consideration for many patients. It also tends to be more cost-effective compared to implants, while maintaining the natural feel and function of the tooth.
From a functional standpoint, a natural tooth — even when restored — behaves differently from an artificial replacement. It remains connected to the surrounding ligament, allowing it to respond to pressure and adapt over time.
This contributes to a more natural chewing experience and better long-term comfort.
That said, it is equally important to recognise that not every case is suitable for avoiding tooth extraction. In situations where the root is compromised, bone support is inadequate, or infection is uncontrolled, proceeding with tooth extraction is the right and responsible decision.
The goal is not to avoid tooth extraction at all costs, but to ensure that it is recommended only when truly necessary.
This is where careful diagnosis and patient-centered decision-making become essential.
At our clinic, when a patient comes in after being advised tooth extraction, we begin by reassessing the case in detail.
The intention is not to challenge previous recommendations, but to confirm whether tooth extraction is necessary or if there is still a possibility to preserve the natural tooth.
In many cases, extraction remains the best option. But in some, we find that the tooth can still be saved — and those are the cases where a different outcome becomes possible.
This approach is closely aligned with how we evaluate other treatments, such as root canal therapy. Just as not every painful tooth requires a root canal, not every damaged tooth requires tooth extraction.
The decision always comes down to accurate diagnosis and understanding the true condition of the tooth.
For patients, this distinction can make a significant difference.
Because choosing between tooth extraction and saving a natural tooth is not just about addressing the immediate problem.
It is about making a long-term decision that affects oral health, comfort, and confidence.
If you have been advised tooth extraction, it may very well be the correct recommendation. But it is always worth asking one important question:
Is tooth extraction the only option, or can this tooth still be saved?
Because in some cases, with the right approach, it is possible to avoid tooth extraction and preserve the natural tooth — and that possibility is always worth exploring.
Case#197: When a tooth extraction was advised, but we saved it.
Patient ID: TD1477 | Tooth 45
Patient symptoms: a broken tooth that seemed beyond saving
The patient presented with a severely broken tooth in the lower right region. By the time they visited us, the visible portion of the tooth had almost completely fractured, leaving behind only a root stump at the gum level.
Functionally, the tooth was no longer usable, and eating on that side had become uncomfortable.
Over time, the condition had worsened gradually. What initially started as mild discomfort had progressed into a structural breakdown of the tooth.
The patient was concerned not just about function, but also about whether the tooth could be saved at all.
Before coming to us, they had already consulted multiple clinics. The recommendation was consistent across all consultations:
Tooth extraction, followed by replacement with an implant or bridge.
Although the patient understood the reasoning behind this advice, they wanted clarity on one important question:
Can tooth extraction be avoided, or is there a way to save this broken tooth? If you’ve been told that your tooth cannot be saved and needs extraction, your situation may be very similar to this case.
Diagnosis findings: what the X-ray revealed beyond the surface
While the clinical appearance suggested that tooth extraction was the only option, a detailed evaluation told a different story.
The tooth had already undergone root canal treatment in the past, which meant that internal infection had been addressed earlier.
The next step was to evaluate the condition of the root and surrounding bone.
An X-ray was taken to assess the deeper structures.
The findings were critical.
There were no periapical changes, indicating that there was no active infection at the root tip. The surrounding bone support was adequate, and the root length was intact — long enough to support a restoration.
This was not obvious from the external appearance.
Because even though the crown was lost, the foundation of the tooth remained stable.
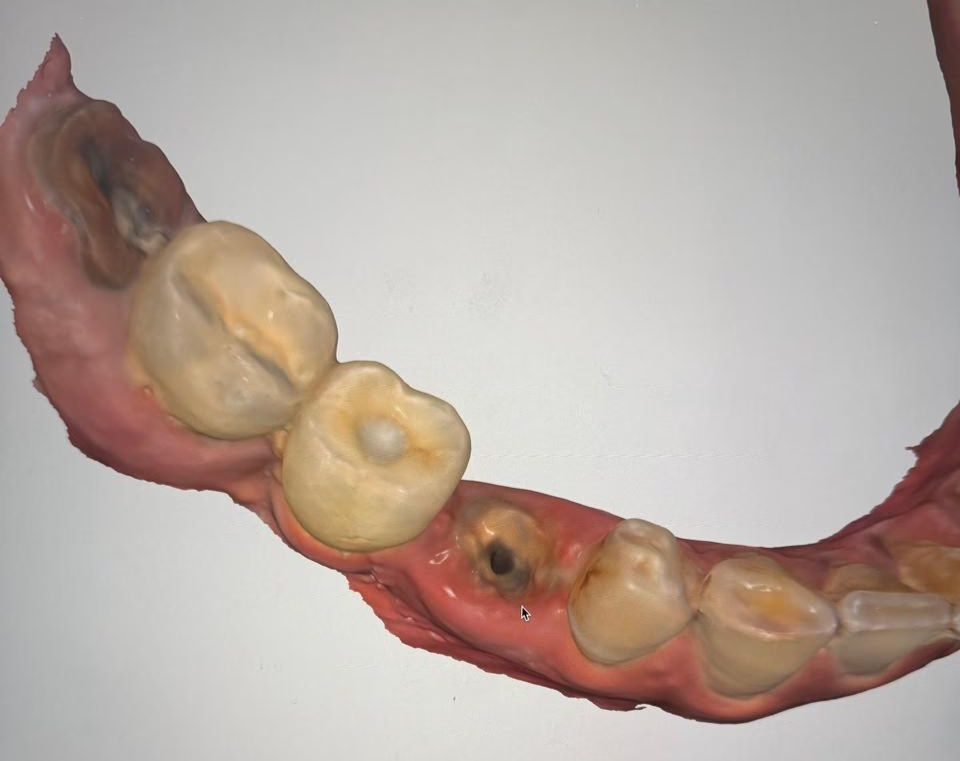
X-ray showing intact root structure (no infection)
Many patients who come to us at this stage have already been told that tooth removal is the only option. In some cases, that is true. But in others, as seen here, the tooth may still be saved.
This is where many patients realise that what appears to require tooth extraction may still be saved.
The turning point: when tooth extraction may not be necessary
This was the stage where the treatment direction changed.
Tooth extraction is usually recommended when the tooth is structurally compromised and cannot be restored predictably.
However, in this case, the absence of infection and the presence of a stable root created an opportunity.
Could this tooth be saved without tooth extraction?
A healthy root provides the possibility of rebuilding the tooth rather than removing it.
After discussing the findings in detail, including the guarded prognosis and long-term considerations, the patient chose a conservative approach.
The decision was not about avoiding tooth extraction blindly, but about choosing an alternative to tooth extraction where clinically appropriate.
The difference between removing a tooth and saving it often lies in a detailed diagnosis — something that is not always explored fully in the first consultation.
A treatment decision focused on avoiding tooth extraction
At this stage, two clear options were available.
One was to proceed with removal and replace the tooth with an implant or bridge. This remains a reliable and commonly recommended solution in such cases.
The other option was to preserve the natural tooth using a post, core, and full-coverage crown.
Choosing to save the tooth offered several advantages. It avoided surgical intervention, preserved the surrounding bone, and was more cost-effective compared to an implant.
Most importantly, it allowed the patient to retain their natural tooth.
This approach aligned with a broader principle in dentistry:
Preserve the natural tooth whenever it is clinically possible to do so.
Treatment done: rebuilding a broken tooth without extraction
The treatment began with local anesthesia to ensure a completely comfortable procedure.
The surrounding soft tissue was carefully managed to expose the root margin, allowing proper access to the remaining tooth structure.
The next step involved preparing the internal structure of the tooth.
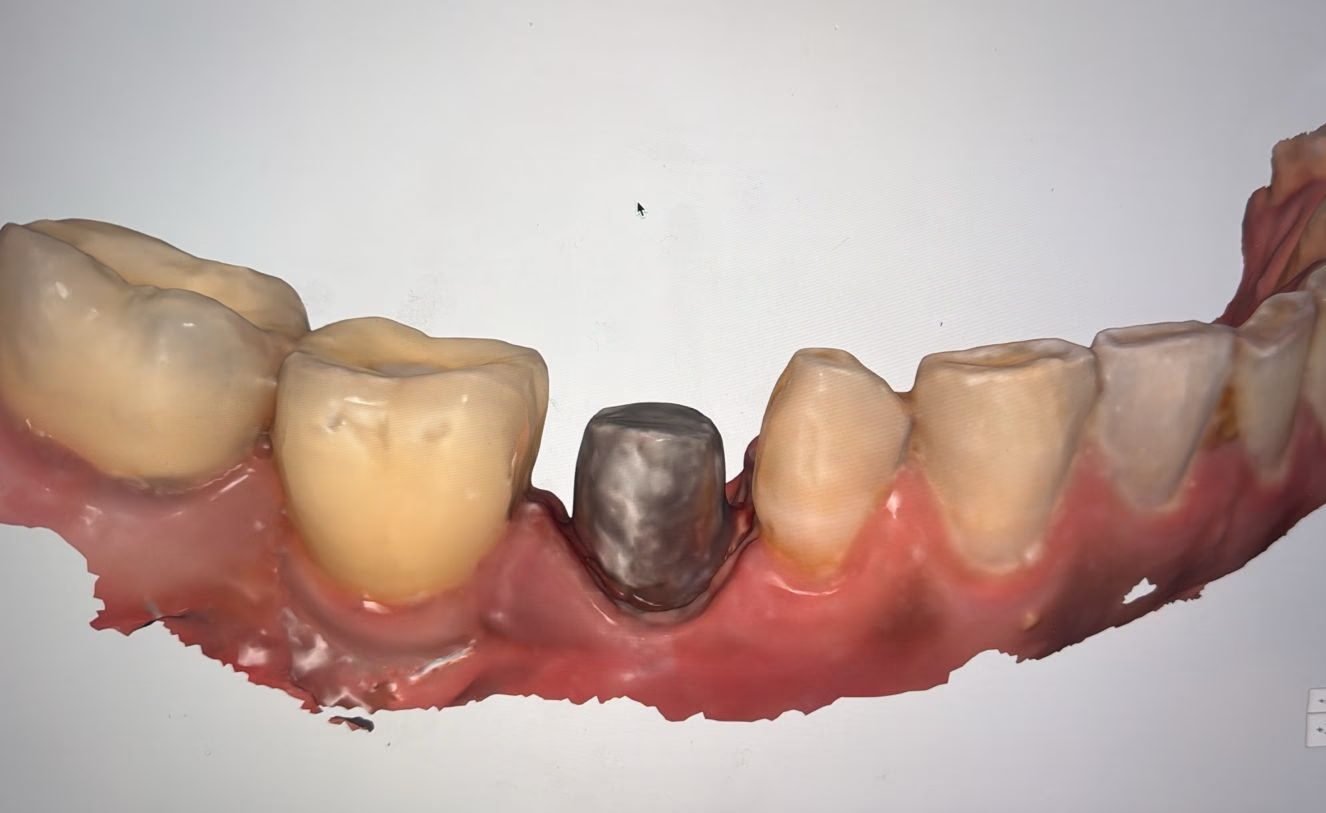
A post space was created within the existing root canal. This space would accommodate a customized post, which acts as a reinforcement and provides retention for rebuilding the tooth.
A digital scan was taken to design a custom post and core, ensuring precise adaptation to the root canal.
Once fabricated, the post and core were cemented securely, creating a stable internal foundation.
At this stage, the tooth — which initially appeared non-restorable — had regained structural support.
Advanced restoration: strengthening the tooth for long-term function
With the internal foundation in place, the focus shifted to strengthening the tooth externally.
The Biologically Oriented Preparation Technique (BOPT) was used to prepare the tooth. This technique is particularly useful in compromised teeth, as it allows better adaptation of the crown and improves long-term stability.
The tooth was then digitally scanned again to fabricate a full-coverage crown using CAD/CAM technology. This ensures precision, durability, and proper fit.
Within a few days, the crown was ready and cemented securely.
At this point, the tooth had been fully restored — both structurally and functionally.
Outcome: saving a natural tooth instead of extraction
Following the treatment, the patient experienced complete functional rehabilitation. The tooth was stable, chewing function was restored, and there was no discomfort.
From a clinical standpoint, the restoration demonstrated good retention and stability.
From the patient’s perspective, the outcome was even more meaningful:
Tooth extraction was successfully avoided.
The natural tooth was preserved.
This case highlights an important takeaway for patients who are advised tooth extraction.
Not every broken tooth requires removal.
With proper diagnosis and the right approach, it is sometimes possible to save a broken tooth without removal and achieve a stable, long-term result.
Tooth extraction vs saving the natural tooth — what patients should know before deciding
This case brings out a very important principle in dentistry — and one that every patient should clearly understand before proceeding with the removal of the complete tooth.
Not every severely damaged tooth needs to be removed.
In many situations, especially where the root remains healthy and the supporting bone is intact, it is possible to avoid complete removal and restore the tooth using conservative techniques.
With proper diagnosis, careful treatment planning, and the right clinical approach, dentists can often save a broken tooth without extraction, even when it appears unsalvageable at first glance.
This is where the idea of an alternative to complete removal becomes relevant.
Patients are often advised extraction based on how the tooth looks clinically — for example, when only a root stump remains. However, the decision should not be based only on what is visible.
The true condition of the rootand surrounding bone, and the presence or absence of infection, play a far more important role in determining whether complete removal is necessary.
When these underlying factors are favourable, preserving the natural tooth can offer several long-term advantages.
Avoiding complete removal helps maintain the surrounding bone, reduces the need for surgical procedures such as implants, and retains the natural biomechanics of the mouth.
A natural tooth, even when restored, continues to function in a way that artificial replacements cannot fully replicate.
However, it is equally important to understand the other side of this decision.
There are cases where tooth extraction is the only safe and predictable option. If the root is fractured, if bone support is significantly compromised, or if infection has spread in a way that cannot be controlled, attempting to save the tooth may lead to repeated failure and complications.
In such situations, delaying tooth extraction can actually worsen the condition and increase the complexity of future treatment.
This is why the goal is not simply to avoid tooth extraction at all costs.
The goal is to ensure that tooth extraction is done only when it is truly necessary — and avoided when a reliable alternative exists.
This balance is very similar to how we approach root canal treatment decisions. Just as not every painful tooth requires a root canal, not every damaged tooth requires extraction.
In both cases, the decision depends on accurate diagnosis, clinical judgment, and a patient-first approach.
For patients, this distinction is extremely important.
Because choosing between tooth extraction and saving a natural tooth is not just about addressing the immediate problem.
It is a long-term decision that affects oral health, function, comfort, and overall confidence.
If you have been advised tooth extraction, it may very well be the correct recommendation. But it is always worth asking one important question:
Is tooth extraction truly necessary in this case, or can the tooth still be saved?
Because in some cases, with the right evaluation and treatment, it is possible to avoid tooth extraction and preserve what you already have — and that possibility is always worth exploring.
Why a second opinion can make a difference before tooth extraction
When patients are advised tooth extraction, the recommendation often feels final.
The assumption is that the tooth cannot be saved and that removal is the only safe option. In many cases, that advice is absolutely correct.
But in some situations, especially when the condition of the root and supporting structures has not been fully evaluated, there may still be an opportunity to avoid complete removal.
This is where a second opinion becomes valuable.
Seeking another evaluation is not about doubting or challenging the first dentist’s recommendation. Dentistry, like all areas of healthcare, involves clinical judgment.
Two experienced clinicians may look at the same case and approach it from slightly different perspectives — particularly in borderline situations where the decision lies between tooth extraction and saving the natural tooth.
A second opinion allows the case to be reassessed with fresh eyes.
In many instances, the original recommendation for tooth extraction is confirmed, and patients can proceed with greater confidence, knowing that the decision is well-founded.
But in some cases, a more detailed evaluation — including X-rays, assessment of bone support, and analysis of root integrity — may reveal that the tooth still has the potential to be restored.
This is especially relevant in cases where patients are looking for an alternative to tooth extraction, or where the visible condition of the tooth appears worse than the actual underlying foundation.
As seen in this case, even when a tooth looks severely compromised, the presence of a healthy root and adequate bone support can open the possibility to save a broken tooth without extraction.
A second opinion also creates space for a more detailed discussion.
Patients often benefit from understanding not just what is being recommended, but why. When options are explained clearly — including the risks, benefits, and long-term outcomes — it becomes easier to make an informed decision.
In some cases, this may reinforce the need for tooth extraction. In others, it may highlight a conservative approach that was not initially considered.
Importantly, the goal is never to delay necessary treatment.
If tooth extraction is truly required, postponing it can lead to worsening infection, bone loss, or additional complications. A second opinion should not be used to avoid treatment, but to ensure that the treatment being chosen is the most appropriate one for that specific case.
For many patients, this additional step provides clarity and reassurance.
Because the decision between extracting a tooth and preserving it is not just a clinical one — it is also personal. It affects long-term oral health, comfort, and confidence.
Taking the time to explore whether it can be avoided helps ensure that no viable option is overlooked.
And in some cases, that single step — seeking a second opinion — can make the difference between removing a tooth and successfully saving it.
If you’ve been advised to undergo tooth removal and are unsure, it may be worth getting a clear evaluation before proceeding.
Before you decide on tooth extraction
If you have been advised an extraction procedure, it may very well be the correct and necessary decision. In many situations, removing the tooth is the safest way to eliminate infection, relieve pain, and prevent further complications.
But before proceeding, it is important to pause and ask a simple yet powerful question:
Is it truly the only option, or can this tooth still be saved?
This question matters because not every damaged tooth is beyond recovery. In some cases, what appears to be a situation requiring immediate removal of tooth may still have the potential for a more conservative solution.
With a detailed evaluation — including X-rays, assessment of bone support, and examination of the root structure — it is sometimes possible to identify an alternative.
For example, even when a tooth is severely broken, if the root remains intact and the surrounding bone is healthy, it may be possible to save the natural tooth without extraction.
Techniques such as post and core restorations followed by a full-coverage crown can rebuild the tooth and restore function. These approaches are designed to preserve what remains, rather than remove it.
This does not mean that tooth extraction should be avoided in every case.
There are situations where tooth removal is necessary — especially when the root is fractured, bone support is insufficient, or infection has progressed beyond control.
In such cases, delaying extraction can lead to worsening pain, additional damage, and more complex treatment later.
The goal is not to avoid tooth removal at all costs, but to ensure that it is done only when there is no reliable way to save the tooth.
Understanding this balance is important for every patient.
Choosing between an extraction procedure and saving the natural tooth is not just about addressing an immediate dental issue. It is a long-term decision that affects oral health, function, and overall comfort.
A natural tooth, even when restored, continues to maintain bone, support surrounding structures, and provide a more natural chewing experience compared to an artificial replacement.
This is why, before proceeding with the treatment, it is always worth taking that extra step.
Ask your dentist about all available options. Understand the condition of the tooth, the feasibility of saving it, and the long-term outcomes of each approach.
If needed, consider a second opinion to confirm whether tooth removal can be avoided in your case.
Because in certain situations, with the right diagnosis and treatment plan, it is possible to avoid the removal of tooth and preserve your natural tooth.
And when that possibility exists, it is always worth exploring.
While saving a natural tooth is always preferred, there are situations where tooth extraction becomes necessary.
In such cases, the next decision becomes equally important — how to replace the missing tooth effectively.
What are the options after tooth extraction, and how to choose the right one
If a tooth removal is truly necessary, the next decision becomes equally important: how to replace the missing tooth in a way that restores function, maintains bone, and preserves long-term oral health.
Many patients focus only on removing the painful or damaged tooth. But what happens after tooth extraction has a direct impact on chewing ability, alignment of surrounding teeth, facial structure, and even future treatment complexity.
This is why it is important to understand the available options before or soon after proceeding with a tooth extraction.
The right choice depends on your specific condition — and a detailed evaluation helps you decide with clarity.
Why replacing a tooth after extraction matters
When a tooth is removed and not replaced, the surrounding bone in that area gradually begins to shrink. This process, known as bone resorption, can affect both function and appearance over time.
Adjacent teeth may begin to shift into the empty space, leading to misalignment and bite changes. Opposing teeth may also over-erupt, creating further imbalance.
Replacing the tooth after extraction helps:
- maintain bone structure
- preserve alignment of nearby teeth
- restore chewing efficiency
- prevent long-term complications
This is why, in most cases, dentists recommend a replacement plan after tooth extraction.
Dental implants — the closest alternative to a natural tooth
A dental implant is often considered the most advanced and long-term solution after tooth removal. It involves placing a titanium post into the jawbone, which acts as an artificial root.
A crown is then placed on top, restoring both function and appearance.
The key advantage of implants is that they mimic the natural tooth structure, including the root.
This helps maintain bone levels and provides a stable, independent replacement without affecting adjacent teeth.
However, implants do require:
- sufficient bone support
- a minor surgical procedure
- healing time before final restoration
They are also relatively higher in cost compared to other options, but offer excellent long-term outcomes when done correctly.
Dental bridge — a fixed solution using adjacent teeth
A dental bridge is another commonly used option after tooth extraction. In this approach, the missing tooth is replaced by a prosthetic tooth that is supported by the adjacent teeth on either side.
This option does not require surgery and can be completed relatively quickly. It restores function and aesthetics effectively, especially when the adjacent teeth already require crowns.
However, it does involve preparing the neighbouring teeth, which means altering otherwise healthy tooth structure. Additionally, it does not replace the root, so it does not prevent bone loss in the extracted area.
Partial denture — a removable and economical option
For some patients, especially when multiple teeth are missing, a removable partial denture may be considered after tooth extraction.
This is a more economical option and can restore basic function and appearance.
While dentures can be useful in certain situations, they may not provide the same level of stability or comfort as fixed solutions like implants or bridges.
They also require regular maintenance and adjustment over time.
Can you choose not to replace a tooth after extraction procedure?
In some cases, patients consider not replacing the tooth after tooth extraction, especially if the missing tooth is not visible or does not immediately affect function.
While this may seem acceptable in the short term, it often leads to gradual changes in the mouth. Bone loss, shifting of teeth, and bite imbalance can develop over time, making future treatment more complex.
This is why, even if replacement is delayed, it is important to plan for it.
Making the right decision after tooth removal
Choosing the right option after tooth extraction depends on several factors:
- the location of the missing tooth
- the condition of surrounding teeth
- available bone support
- overall oral health
- patient preference and budget
There is no one-size-fits-all solution. The best approach is one that balances function, longevity, and patient comfort.
A final perspective: preserve when possible, replace when necessary
While modern dentistry offers multiple ways to replace a tooth after extraction, it is important to remember that no replacement can fully replicate a natural tooth.
This is why, whenever possible, the first goal is always to save the natural tooth and avoid the extraction procedure.
But when extraction becomes necessary, choosing the right replacement ensures that oral health and function are maintained effectively.
If you have been advised tooth removal, it is helpful to discuss not just the removal of the tooth, but also the plan for what comes next.
A well-thought-out approach after extraction can make a significant difference in long-term outcomes.
In many cases, patients proceed with tooth extraction without realising that alternatives may exist — taking a moment to explore those options can make a lasting difference.
Common questions about Tooth Extraction
Can tooth extraction be avoided?
In some cases, yes — the extraction procedure can be avoided if the tooth’s root is still healthy and there is adequate bone support. Even when a tooth appears severely damaged, it may be possible to save the natural tooth without extraction using treatments such as a post-and-core with a crown. However, this depends entirely on proper diagnosis, including X-rays and clinical evaluation.
Is a broken tooth always removed?
No, a broken tooth does not always require removal of tooth. If the damage is limited to the visible portion and the root is intact, the tooth can often be restored. Many patients are surprised to learn that it is possible to save a broken tooth without extraction, depending on the condition of the root and surrounding bone.
When is tooth extraction necessary?
Tooth removal is necessary when the tooth cannot be restored predictably. This includes cases with severe root fractures, advanced bone loss, or uncontrolled infection. If saving the tooth would lead to repeated failure or complications, extraction becomes the safest and most reliable option.
What are the alternatives to tooth extraction?
Alternatives to tooth removal depend on the condition of the tooth. If the root is healthy, options may include rebuilding the tooth using a post and core, followed by a crown. These treatments aim to avoid tooth removal and preserve the natural tooth. However, not all cases are suitable for this approach.
How do I know if my tooth can be saved instead of extraction?
The only way to determine this is through a detailed dental evaluation. Your dentist will assess X-rays, root condition, bone support, and infection levels. If these factors are favourable, it may be possible to avoid losing the tooth and instead restore it. Seeking a second opinion can also help in making a more informed decision.
Is it better to save a natural tooth or replace it after extraction?
Whenever possible, it is generally better to save the natural tooth instead of extraction. A natural tooth helps maintain bone, supports surrounding structures, and provides a more natural chewing experience. However, if the tooth cannot be saved reliably, removing the tooth followed by replacement (such as an implant) becomes the better option.
Should I take a second opinion before tooth extraction?
Yes, taking a second opinion before removing a tooth can be helpful, especially in borderline cases. Another evaluation may confirm what is necessary or reveal an alternative to extraction that allows you to preserve your natural tooth. The goal is to ensure that all possible options have been explored before making a final decision.
Advised a Root Canal Treatment? We saved the tooth without it.
Learn more from Happy Patient Reviews.
The True Cost of Dental Implants in India (2026).
The True Cost of Tooth Crowns in India (2026).
Why patients trust The Dentist
At The Dentist, our philosophy is built around Ethical & Conservative Dental Care.
Whether you’re a local patient, an expat in India, an NRI, or an international traveller seeking advanced dental treatment, our focus is the same: preserve natural teeth whenever possible, recommend only necessary treatment, and deliver dentistry designed for long-term comfort, function, and oral health.
Over the years, patients from India and across the world have trusted The Dentist for Root Canal Treatment, Dental Crowns, Smile Rehabilitation, Dental Implants, Cosmetic Dentistry, and full-mouth restorative care because of our emphasis on transparency, precision, and conservative treatment planning.
Conservative dentistry before aggressive treatment
We strongly believe that nothing functions quite like your own natural teeth. Whenever possible, our approach focuses on preserving healthy tooth structure rather than recommending unnecessary extractions or overly aggressive procedures. Every treatment plan is designed with long-term oral health and tooth preservation in mind.
Ethical and transparent treatment planning
Patients are carefully guided through available treatment options, expected timelines, advantages, limitations, and estimated costs before treatment begins. Rather than rushing patients toward a single procedure, the focus remains on helping them make informed and comfortable long-term decisions about their oral health.
Advanced technology with precision-focused dentistry
Modern dentistry depends heavily on accuracy and precision. The Dentist uses advanced diagnostic systems, digital scans, precision instruments, and modern restorative workflows designed to improve treatment quality, aesthetics, bite accuracy, comfort, and long-term durability.
Experienced clinicians across major dental specialties
The Dentist brings together experienced clinicians across Root Canal Treatment, Dental Implants, Smile Rehabilitation, Cosmetic Dentistry, Invisible Aligners, and Restorative Dentistry. This multidisciplinary approach allows patients to receive more coordinated and comprehensive treatment planning under one roof.
Premium materials and trusted dental laboratories
The long-term success of treatments such as Dental Crowns, Veneers, Bridges, and Implant restorations depends heavily on material quality and laboratory precision. We work with trusted dental laboratories and premium restorative systems to help ensure natural aesthetics, precise fit, strength, comfort, and longevity.
Focus on long-term comfort and natural function
Good dentistry should not simply look aesthetic initially — it should feel natural and function comfortably for many years. Special emphasis is placed on bite balance, gum health, precision fit, chewing comfort, and long-term oral stability across all treatments.
Strict sterilisation and patient safety protocols
Patient safety remains a core priority at every stage of treatment. The clinic follows strict sterilisation and hygiene protocols designed to maintain high standards of infection control, cleanliness, and procedural safety.
Personalised care for local and international patients
Whether treating a local family from Delhi, an expat working in India, or an international patient visiting for advanced dental treatment, every patient receives detailed evaluation, personalised treatment planning, and dedicated attention. We strongly believe that quality dentistry requires time, communication, and individualised care rather than rushed consultations or standardised treatment approaches.
Trusted by patients from India and around the world
Over the years, patients from the United States, United Kingdom, Europe, Australia, the Middle East, Africa, and Asia have visited The Dentist for advanced restorative and cosmetic dental care. Many international patients appreciate the combination of ethical treatment planning, conservative dentistry, advanced technology, personalised communication, and efficient treatment coordination available at the clinic.
Dentistry designed for long-term oral health
Ultimately, our philosophy is simple — deliver dental treatment that preserves natural teeth whenever possible, functions comfortably, looks natural, and remains stable for many years to come.

